Is Deep Vein Thrombosis Life-Threatening?
Yes, Deep Vein Thrombosis (DVT) can be life-threatening if left untreated. Blood clots formed in deep veins, typically in the legs, can break free and travel to the lungs, causing a pulmonary embolism—a potentially fatal condition.
Characteristics of Deep Vein Thrombosis (DVT)
- Chronic leg swelling.
- Pooling of blood in veins.
- Increased skin discoloration or pigmentation.
- High pressure within the veins.
- Venous stasis ulcers (leg ulcers caused by poor blood flow).

Common Symptoms of DVT
- Pain or tenderness in the affected arm or leg, often while walking or standing.
- Sudden swelling in an arm or leg.
- Warmth in the swollen or affected area.
- Enlarged veins visible near the skin’s surface.
- Severe headaches or seizures (if clots affect brain veins).
- Flank or abdominal pain (if clots affect deep abdominal veins).
Causes of DVT
- Genetic Factors: Family history of DVT or clotting disorders.
- Medical Conditions: Cancer, obesity, or recent surgery.
- Immobility: Prolonged sitting, bed rest, or immobilization.
- Pregnancy: Hormonal changes and pressure on veins increase the risk.
- Lifestyle: Smoking, hormone therapy, or birth control pills.
- Infections: Severe cases of COVID-19.
- Age: Increased risk as you get older.
Diagnosing DVT
- Duplex Venous Ultrasound: A non-invasive test using ultrasound waves to detect clots and measure blood flow.
- Venography: Rarely used; involves injecting contrast dye to highlight clots on X-rays.
- Magnetic Resonance Imaging (MRI) or Magnetic Resonance Venography (MRV): Advanced imaging techniques to locate blood clots.
- CT Scan: Used for identifying DVT in the abdomen, pelvis, or brain.
Treatment for Deep Vein Thrombosis
The primary goals of DVT treatment include:
- Preventing Clot Growth: Using anticoagulants (blood thinners).
- Avoiding Clot Dislodgement: Preventing it from traveling to the lungs.
- Reducing Recurrence Risk: Encouraging regular movement and compression therapy.
- Managing Long-Term Effects: Preventing chronic venous insufficiency or post-thrombotic syndrome.
What Is Deep Vein Thrombosis?
Deep vein thrombosis also known as venous thrombosis; occurs when a thrombus (blood clot) is formed in the veins deep in an individual’s anatomy because the veins of an individual are damaged, or the blood streaming by them is too sluggish. The thrombus may entirely or partially jam the blood streaming of an individual’s vein. Deep vein thrombosis mostly happens in the lower leg, pelvis or thigh, but there are chances that they also occur in other body parts like the arm, intestines, brain, kidney, or liver.Is Deep Vein Thrombosis Life-Threatening?
The deep vein thrombosis itself is not severe; the blood clots have the potential to break free and travel through an individual’s blood flow. A PE (pulmonary embolism) happens when the traveling blood clots known as emboli become lodged in the blood vessels of an individual’s lungs. Pulmonary embolism can be a life-threatening disorder. The individual is advised to visit the health care provider for the diagnosis and medication. Most individuals diagnosed with deep vein thrombosis are likely to develop symptoms of intermittent leg swelling and discomfort that can last longer. The indications of deep vein thrombosis are called post-thrombotic syndrome and can occur due to damage to the valves and inner lining of an individual’s vein leading to blood “pooling” more than it should be. The rise in the pressure inside the individual’s veins leads to swelling and pain.The Characteristics Of Deep Vein Thrombosis Include:
- Chronic leg swelling.
- Pooling of blood.
- Increased discoloration or pigmentation of the skin.
- Increased pressure within the veins of an individual.
- Leg ulcers are known as venous stasis ulcers.
How Common Is Deep Vein Thrombosis?
Every year almost one to three in every one thousand individuals are diagnosed with deep vein thrombosis or (PE) pulmonary embolism. In the U.S., nearly 300,000 individuals die yearly due to (PE) pulmonary embolism or deep vein thrombosis. Behind heart attack and stroke, deep vein thrombosis is the third most common disorder. An acute PE/DVT can happen at any age and is more common in individuals over sixty. The cause why DVTs are common in hospitals is because the patient is lying in bed most of the time instead of making any movement.What Are The Indications Of Deep Vein Thrombosis?
Deep vein thrombosis typically happens in the veins of an individual’s arms or legs. Most individuals encounter mild or no symptoms and may not raise concern. Following are the symptoms of deep vein thrombosis:- Tenderness or pain in an individual’s arm or leg. The discomfort usually occurs while walking or standing.
- Sudden swelling of arm or leg.
- The swollen or hurt area of an individual’s leg or arm may feel warmer than usual.
- The veins near an individual’s skin’s surface may be larger than usual.
- Severe headaches or seizures when the blood clots affect the veins of an individual’s brain.
- Flank pain or abdominal pain is when the blood clots affect the veins deep inside an individual’s abdomen.
What Are The Causes Of Deep Vein Thrombosis?
Following are the health conditions that can cause deep vein thrombosis in an individual:- Having cancer and cancer treatments like chemotherapy.
- Having a genetic disorder that increases the risk of blood clots.
- Having a medical background of deep vein thrombosis in the family.
- Not able to move the body for a longer time, like sitting, for an extended period.
- Having limited bloodstream in a deep vein due to an injury, immobilization, or surgery.
- Being pregnant or recently delivered a baby.
- Being obese and aging.
- Consuming tobacco products.
- Having hormone therapy or birth control pills.
- Having COVID-19
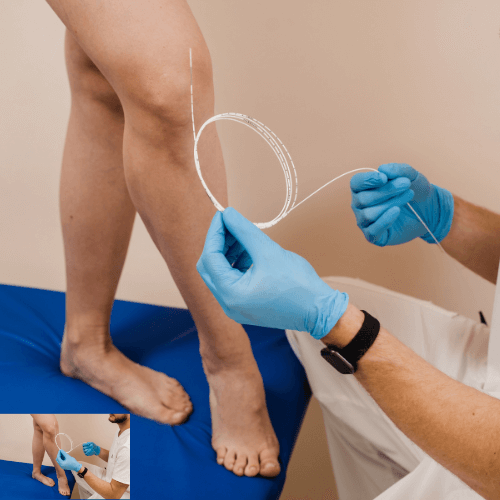
How To Diagnose Deep Vein Thrombosis?
After analyzing the symptoms and conditions of an individual, the healthcare advisor can ask for the following imaging tests:- Duplex venous ultrasound: This is a non-invasive and widely available test to diagnose deep vein thrombosis. In this examination, the consultant will use ultrasound waves to show blood streaming and blood clots in an individual’s veins.
- Venography: In this test, the healthcare advisor will numb the skin of the patient’s neck or groin and utilizes a catheter to inject a special dye known as the contrast material into the veins of an individual to highlight the blood clots blocking blood flow inside an individual’s veins. However venography is rarely used presently, but it can become necessary according to the patient’s situation.
- Magnetic resonance venography (MRV) or magnetic resonance imaging (MRI):
- (CT) computed tomography scan: shows insight pictures of a patient’s anatomy. The healthcare advisor can suggest a CT scan to locate a deep vein thrombosis in an individual’s abdomen, pelvis, or brain.
What Is The Possible Treatment For Deep Vein Thrombosis?
The treatment for deep vein thrombosis includes medication known as anticoagulants that work as a blood thinner, elevating and stocking the patient’s legs at different times a day. The primary purpose of deep vein thrombosis includes:- Reducing the risk of another blood clot.
- Preventing the clot from involving and getting more prominent in other veins.
- Keep the chunk from breaking off in the patient’s vein and transferring to the patient’s lungs.
- Prevent long-term complications from blood clots, such as chronic venous insufficiency.
References
- https://www.webmd.com/dvt/what-is-dvt-and-what-causes-it retrieved on 1 September 22
- https://www.healthline.com/health/deep-venous-thrombosis retrieved on 1 September 22
- https://my.clevelandclinic.org/health/diseases/16911-deep-vein-thrombosis-dvt retrieved on 1 September 22
- https://www.mayoclinic.org/diseases-conditions/deep-vein-thrombosis/symptoms-causes/syc-20352557#:~:text=Deep%20vein%20thrombosis%20(DVT)%20occurs,affect%20how%20the%20blood%20clots. Retrieved on 1 September 22
